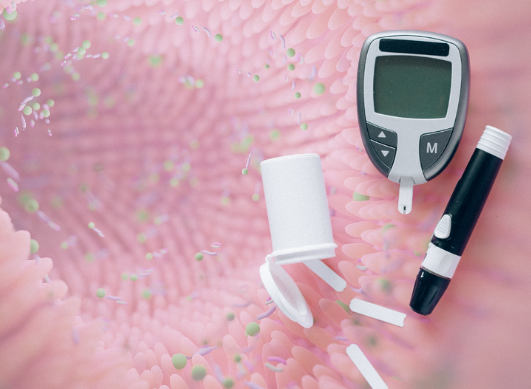
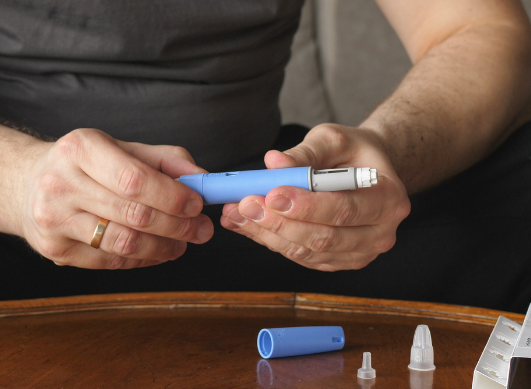
Diabetes (Type 2) Forum
- 3,251 members
- 7 discussions
Post on this group all links, articles or web pages that caught your attention and have to do with the disease (treatment, medical research, therapeutic innovation, seminars on the disease or any event)
Patients Diabetes (Type 2)
Research and useful links - Type 2 Diabetes
Type 2 diabetes: Late breakfast could drive obesity
![]()
![]()
Research and useful links - Type 2 Diabetes
How Cinnamon Lowers Blood Sugar and Fights Diabetes
![]()
![]()
Research and useful links - Type 2 Diabetes
Diabetes type 2 - Not hungry anymore?
![]()
Research and useful links - Type 2 Diabetes
Consuming Milk At Breakfast Lowers Blood Glucose Throughout The Day
![]()
![]()
![]()
Research and useful links - Type 2 Diabetes
Air Pollution Plays Significant Role In Diabetes: Study
Research and useful links - Type 2 Diabetes
Why Lifestyle Changes Won’t Work For Everyone With Type 2 Diabetes
![]()