Melanoma: How do you know if a mole is dangerous?
Published Jun 24, 2020 • By Candice Salomé
We all have many moles on our bodies. Also called nevi, they are most often characterized as small brown spots, raised or flat, and usually appear before the age of 30. Their number on the body depends on certain hereditary factors but also on exposure to the sun. Most of them are not dangerous.
Nevertheless, it is still essential to keep an eye on moles because some could turn into melanoma (a malignant tumor). So, what are the signs that should alert us to a problem?

Adults have on average about twenty moles on their bodies. The parts of the body that are most exposed to the sun tend to have more. For men, these are often the back and for women, the legs.
While moles are harmless, they can change over the course of one's life. It is therefore essential to monitor them regularly.
Why can moles be so dangerous?
Skin cancers are the most commonly occurring cancer in the United States, with more than 9,500 diagnoses made every day.
According to The Skin Cancer Foundation, in the past decade, the number of new invasive melanoma cases diagnosed annually increased by 47%.
This evolution can be explained by increasing trends of sun exposure. Melanoma, if treated late, cannot be cured. For this reason, sun protection measures and early detection are the only ways to reduce the incidence of skin cancer.
Color, size, shape: what are the warning signs?
According to Emmanuel Ricard, delegate for prevention and promotion of screening at the French League Against Cancer (la Ligue contre le Cancer), a mole that changes, spreads or changes color, becomes thicker or rough should be checked immediately.
Furthermore, if you have more than 30 moles, or have already had one removed, it is recommended that you see a dermatologist once a year.
How to distinguish a mole from a developing melanoma?
In 80% of cases, melanoma resembles a mole at the beginning of its development. It is therefore complicated to differentiate a developing melanoma from a recent nevus. In only 20% of cases, the melanoma comes from the malignant transformation of an existing mole.
Is anyone more at risk of developing skin cancer?
Some people are at higher risk of developing skin cancer from a nevus. This may be related to genetic factors (very fair skin, eyes and hair or a family history of melanoma or other skin cancers). Environmental factors can also play an important role (numerous sunburns during childhood or a tendency of over-exposing one's self to the sun).
How to early detect skin cancer yourself?
As skin cancers appear in many shapes and sizes, it is important to be familiar with the warning signs. These characteristics can be easily remembered with the ABCDE rule:
A: for Asymmetry. If you were to draw a line through the center of the mole, the two sides will not match.
B: for Borders. The borders of an early melanoma tend to be uneven, while benign moles tend to have smoother, more even borders.
C: for Color. Multiple colors are a warning sign, as common moles are all one color. Melanoma may have shades of brown, tan or black.
D: for Diameter. Melanomas are usually the size a pencil eraser (about 6 mm) or larger.
E: for Evolving. If you notice changes in shape, size, color, elevation or new symptoms such as itching, bleeding or crusting, it is a warning sign.
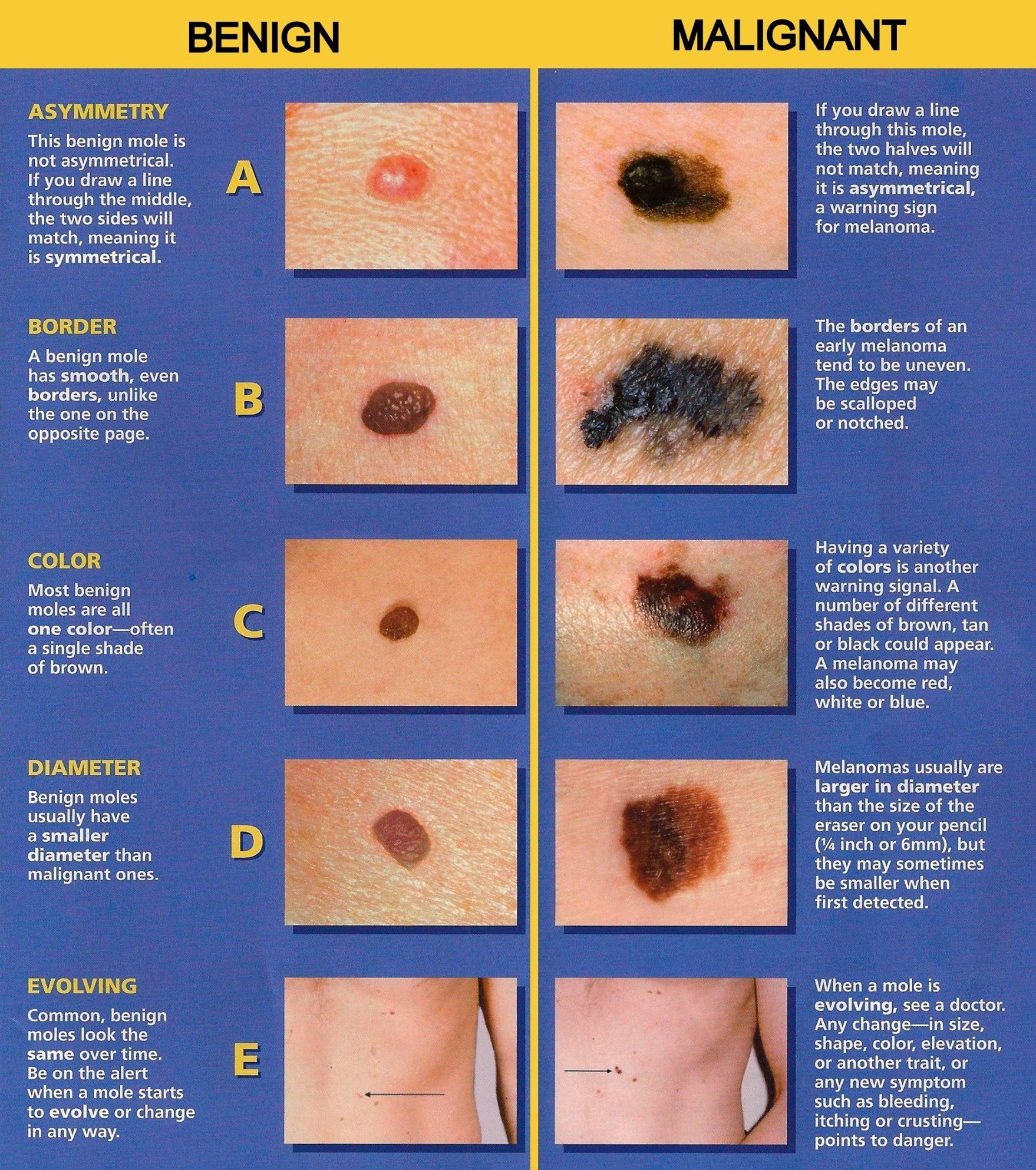
Photo credit: The Skin Cancer Foundation
Biopsy: the key test for diagnosis!
Early melanomas can be difficult to differentiate from an atypical nevus (a melanoma-like mole). If your dermatologist has any doubts, he or she will surgically remove your mole immediately and have it analyzed. The purpose of biopsy is to remove the supposed tumor but also, after examination, to make a diagnosis. It is usually performed under local anesthesia. The removed skin fragment is sent to an anatomical pathologist (a doctor who analyses tissue samples) for microscopic analysis. Study of the sample can confirm (or not) the malignant nature of the mole and will make it possible to diagnose it (or not) as skin cancer.
Please note that any destruction of a mole, whether suspicious or not, for example by laser, is to be avoided because no analysis can be done afterwards.
How is a melanoma removed?
The broad excision of a melanoma is performed under local anesthesia. This operation makes it possible to remove and heal the lesion (most of the time) if it is detected early. This procedure is painless and takes no more than a few minutes.
Additional examinations such as X-rays or ultrasound scans are then required to look for other possible lesions. These examinations make it possible to determine the spread of the melanoma to other parts of the body. Based on these results, the doctor decides whether additional treatment is necessary: removal of a second melanoma, immunotherapy, chemotherapy, etc.
A regular check-up by a dermatologist will be necessary afterwards.
Where can I find a free skin cancer screening?
The American Academy of Dermatology has been periodically organizing free SPOT me® skin cancer screenings across the country since 1985. You can find a free screening in your area by using their online tool here.
Members of the American Society for Dermatologic Surgery also provide free skin cancer screenings. You can find availabilities in your area by using their search tool here.
Was this article helpful to you? Why don't you share your feelings with the community?
Take care!
Comments
You will also like

What are the dangers associated with the over-the-counter sale of certain medicines?
Dec 19, 2020 • 6 comments

 Facebook
Facebook Twitter
Twitter

